

See you there! We will be set up and available for our routine services if needed!


See you there! We will be set up and available for our routine services if needed!

Have you ever thought about acupuncture treatments? Many of our clients are proponents of using this ancient therapy to treat their horses, but they are missing out on the advantages it offers to equestrians. Here at AED, we have all had acupuncture therapies with much success….and we’d like to recommend our clinician!

Do you love riding horses? Do you ever suffer anxiety during a ride or competition? Have you experienced injuries/pain resulting from your riding or training? My name is Dr. Lexy Ballinger and many of the clients in my practice are equestrians. I am honored to be an integral part of their path to improvements in the saddle.
Did you know that acupuncture is an extremely effective treatment for both anxiety and pain? The best part of acupuncture is it can help with many medical conditions without the need to take medications or experience their possible side effects. By accessing acupuncture points, your body is aided in rebalancing and healing itself. In addition to the long, documented history of acupuncture in traditional Chinese medicine, studies by the National Institute of Health (NIH) have clearly demonstrated acupuncture as an excellent and effective tool for treating conditions such as anxiety, all types of pain, insomnia, headaches, migraines, and stress. If you have ever wondered if there was a different way to manage your equine related injuries or a way to facilitate calm during your rides, please call or write to me at (813) 917-1173/ flphoenixrisingacu.com so I may answer your questions! Until then….Happy Riding!

Richard Grist CEqD gets many questions from clients about the tools he chooses to work with and the benefits of those tools to equine dental care. As with anything “horse” related, there are endless opinions and theories passed around and adopted into the health care routines of owners. Follow along as we explain how Advanced Equine Dentistry performs dental care, why we use specific tools and procedures, and the facts behind our expert performance!


One of the first tools you will see used on your horse during a dental visit with AED is a speculum. While the speculum certainly protects the dental practitioner from being injured, its actual use is to protect your horse. Not only can horses be injured from biting down on dental tools, they can also be gravely injured from dental tools being utilized blindly. Imagine your own dentist inserting a long, sharp rasp into your own mouth without being able to see the termination of your teeth or what parts they were actually touching! The speculum, when used properly, holds the equine jaw open so that the dentist can reach every tooth surface and can see every tooth surface. Anatomically, it also creates enough separation of the grinding surfaces of the molars to allow for the removal of any ramps…..if you look at the equine skull, you can see that without opening the horse’s mouth, these final teeth stay in contact and would prevent a thorough dental procedure! It is not uncommon for AED to be called to treat horses who are having riding/bitting/head tossing issues but who have also recently been “floated”. In many of these horses, we find remaining ramps that would have been impossible to access if a speculum was not used in their previous care.
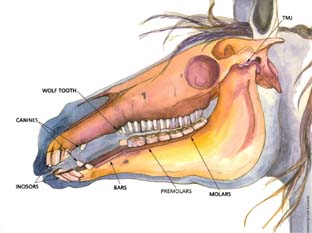
Whether you use Advanced Equine Dentistry or any other dental practitioner, your horse needs you to know that they WANT a speculum used to protect them and to allow for the very best dental procedure! It isn’t torture….it is safety!



It’s Springtime! And along with the return of our awesome weather comes more horse riding, more horse events, more horse shows, more horse everything! Just like we “spring clean” our homes, this month is a great time to make a list of your horse’s wellness needs and get those appointments and exams on your calendar! Take a moment to review when your vaccines were last given, if you’ve checked a fecal egg count recently, the expiration dates of your various supplements and equine medications, when your coggins expires, and of course if your horse is due for dental care! Advanced Equine Dentistry sends visit reminders about 6 weeks before your horse is due for care to enable you to make an appointment that fits into your busy schedule……and into ours! See you soon!

First-time horse buyers are often unsure of what exactly they should be looking for when buying a horse. They may be unfamiliar with horse terminology and what, exactly, owning a horse entails. Even some experienced horse owners still need assistance when purchasing a new horse. If you are new to horses, always take an experienced horse person with you. They will know some things to look for. We’ve compiled a short list of things to consider when going to see a potential horse.
1. Does the horse have any past issues with colic, lameness, Cushings, etc? And have they had their vaccines/coggins? It is always important to try and get the vet records from any horse you are going to purchase. Some people say they vaccinated the horse themselves but have no proof. Rabies vaccines can only be purchased and given by a veterinarian. It is also good to ask if the horse is on anything for maintenance, such as supplements or joint injections.
2. Request a pre-purchase exam from a third-party veterinarian. Whatever you plan is for your horse, it is important to get a complete and thorough physical exam of the horse before you buy. X-rays of the legs and feet are often included in a pre-purchase exam, as well. It is equally important to have a vet that has a good reputation and is not connected to either the buyer or the seller perform the exam.
3. Have the horse aged by a veterinarian or certified equine dentist. We get clients all the time that ask us to come and confirm a horse’s age before they buy. We have had clients buy a horse, and then find out it is older/younger than what they seller told them once we check them out. One of the most extreme cases we have seen even had papers confirming that the horse was 5 years old. When we opened up his mouth, he was closer to 20 years old. Most sellers will say a horse is between 10-15 years old, even if they aren’t sure.
4. Ask to take the horse on trial for 7-10 days. This will allow you to see how the horse acts and rides outside its home environment. It will also enable you to see if the horse had been sedated when you tried it out on the farm. There are some shady people out there that will drug a horse to make it quieter when people come to try it out. Be sure to get a written agreement for the trial period!
5. Is the horse a good match for the capabilities of the rider? Some people buy a horse just because it’s pretty or flashy. They don’t consider the fact that the horse doesn’t have any training and they won’t be able to handle or ride it without sending it to a trainer. It is always important to consider your own skills and the training of the horse. For example, if you’re just learning how to ride, don’t buy a horse that is green broke and needs more training. Sure, that black horse with 4 white socks in the field my be pretty, but he’s also an unbroke 4-year-old stallion. Not something for an inexperienced or novice owner.
6. ALWAYS budget what it’s going to cost you to keep the horse. Buying the horse is often the least expensive part of horse ownership. You have to consider everything that goes into owning a horse long term. This includes: vet bills, farrier visits every 4-6 weeks, board costs, feed costs, tack, lessons, training, etc. Cheaper services are often not worth the cost of inferior work. A $3,000 horse can easily turn into an $8-10,000 horse by the end of a year. Insurance is a very good option for horse owners to consider. It can help cover the cost of expensive services and emergencies.
The take-home message from all of this is: be sure of what you are buying. All too often, people end up with buyer’s remorse because they didn’t check off all the boxes before signing the check. If you are ever unsure of a horse’s age, don’t hesitate to give us a call! Teeth are our specialty, after all!
Written by: Morgan Bosch, DVM
Advanced Equine Dentistry
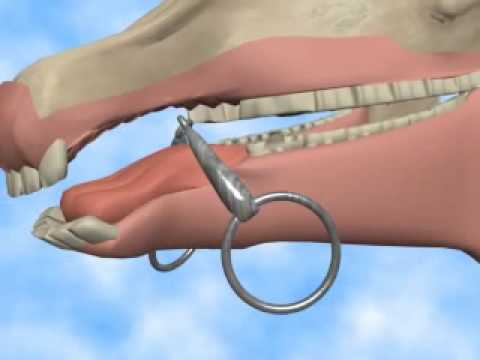
Choosing the right bit size is important. If the bit is either too small or too large it can not do the job it is meant for and can actually harm your horse. Bits, at their best, always create pressure….pressure on soft tissue, on the palate, on the tongue, and even on nerves for the purpose of communication. The very best bit for your horse is the bit with the mildest action while still allowing you a communication pathway. There are many, many, many styles to choose from.
Your horse’s conformation and shape of his mouth/tongue/palate has an impact on what bit will be comfortable for their use. Not all bits fit all horses. Equine dentistry also plays a major role in bit “success” by maintaining the correct alignment and movement of the horse’s jaw. Dentition concerns such as wolf teeth, hooks and ramps, and sharp dental points all can interfere with the movement of their mouth and alter the way a bit actually sits. Finding the right bit for you and your horse may take some trials, but Advanced Equine Dentistry will be happy to assist you by measuring the actual bit seat during your routine dental visit, assessing the conformation of your horse’s tongue and palate, and maintaining their teeth in pristine condition! While we can’t be sure which “bit” you will choose, we can certainly help start your search by giving you some vital information about your horse’s mouth.

Sand colic is a specific type of colic seen in horses that live in a sandy environment. It accounts for about 5% of all colics seen. Sand colic presents with symptoms similar to any generic colic, such as inappetence, pawing, rolling, looking or kicking at the stomach, distress and unease, and dehydration. One sign that is more specific for sand colic is diarrhea. The sand likes to settle in the large colon1, where it causes irritation and pain.


Any equid can pick up sand from the environment. They get it from grazing on sandy pastures, that are often overgrazed by too many horses. Any location with sand is a risk, including if you feed in an arena. They best way to avoid or decrease the risk of your horse ingesting sand is to feed from a rubber tub on the ground for both the hay and the grain. Rubber mats are also an option. This minimizes their exposure to sand and another small particles from the ground. You can also feed from low-hanging hay nets or low mangers.
The way to test for how much sand your horse has is his gut is simple. Take 6 fresh fecal balls that haven’t had contact with the ground and place them in a quart of water in a bucket or bag of some sort. Mix the contents and let sit for 15 minutes. If more than a teaspoon of sand accumulates, your horse is potentially ingesting a dangerous amount of sand1.
There are not a lot of ways to remove the sand, aside from colic surgery. Psyllium is a feed additive that can help move some sand through the gut and out into the feces. If you decide to start adding psyllium, be sure to follow the label instructions for feeding, as it is also a laxative. One veterinarian recommends feeding one to two cups of psyllium per 1,000 pounds of horse daily for a week, every four to five weeks. Alternatively, psyllium can be fed one day a week, every week2. Feeding it every day does not seem to be as effective in clearing the sand from the gut.
If you ever notice signs of colic in your horse, immediately contact your veterinarian. I recommend testing your horses to see how much sand they have in their feces, and then considering adding psyllium to their diet.
Written by: Dr. Morgan Bosch
Works Cited:
1. https://equusmagazine.com/horse-care/the-facts-about-sand-colic-in-horses-8507

For the last 50 years, most horse owners have been told to deworm their horses every 2 months with rotating dewormers. While this has been effective in decreasing infection from what was considered the major parasite of horses 50 years ago, S. vulgaris or the large strongyle, it is now a moot point. S. vulgaris is no longer considered a major player in the parasitic arena in correctly managed herds. Currently, small strongyles called cyanthosomes, Parascaris equorum or equine roundworms, and A. perfoliata or equine tapeworms, are considered the main parasitic threats to equine health1. Due to the extensive use of rotating dewormers, there is emerging drug resistance in many of these parasites, meaning current dewormers aren’t as effective. If horse owners continue to deworm every 2 months, we may soon run out of effective dewormers.
Small strongyles infect almost every horse with access to grass, so it’s important to know how heavy an individual’s parasite burden is. Each horse has some innate resistance to parasites, but it varies from horse to horse. Small strongyles only cause disease when present in large numbers in the horse’s GI tract1. This means that your horse could have a small parasite burden and be perfectly fine. It has been found that in most herds, 15-30% of the horses are responsible for up to 80% of the parasite egg burden1. The main goal of deworming is to target these horses and get their parasite burden down to a manageable level.
So, what should you do? The only way to determine how heavy your horse’s worm burden is is to perform a Fecal Egg Count. This is a test that quantifies how heavy your horse’s infection is, and establishes a baseline to determine treatment. Low shedders have less than 200 eggs per gram of feces. These horses don’t generally require treatment. Moderate shedders have 200-500 EPG, and high shedders have over 500 EPG. These two groups should be treated based on the type of worm present and the type of dewormer those worms are susceptible to. Ideally, the test should be performed prior to deworming, or at least 6 weeks after deworming.
There are several other things you can do to help decrease the egg burden on your farm, such as rotating pastures, removing manure frequently from pastures (at least twice weekly), harrowing/dragging and mowing pastures to expose larvae and eggs to elements and predators, and avoiding equine overcrowding. Florida has different recommendations for deworming due to its climate. The best time to treat horses is during the winter. Below is a chart put together by AED to help aid in deworming your horse with the correct products at the correct time of year based on their Fecal Egg Count test results. If you have any questions, don’t hesitate to ask during our next visit!
Written by: Morgan Bosch, DVM

References
1. AAEP Internal Parasite Control Guidelines. https://aaep.org/sites/default/files/Documents/InternalParasiteGuidelinesFinal5.23.19_0.pdf

Advanced Equine Dentistry would like to wish all of our clients and their amazing horses a wonderful holiday season! Let’s hope the new year will bring us all good health, safety, stability, and JOY!!!